
Introduction
Healthcare organizations are running out of time to fix their hiring. The U.S. faces a projected shortage of 141,160 physicians by 2038 and 108,960 registered nurses by the same year, according to the Health Resources and Services Administration. With a current RN vacancy rate of 9.6% nationally, the gap between demand and available talent keeps widening.
When candidates are scarce, slow hiring processes don't just cause inconvenience — they cost organizations the talent they can't afford to lose. Every unfilled role carries direct costs, averaging $61,110 per bedside RN turnover. Filling an experienced RN position takes 83 days on average — nearly twice the 45-54 day benchmark across other industries. The toll on patient outcomes and staff morale is real.
This article breaks down the most effective strategies healthcare organizations are using to hire faster, reduce costs, and build more resilient teams.
TLDR
- Healthcare hiring complexity stems from credential requirements, compliance obligations, and multi-stakeholder approval chains
- Front-loaded screening, proactive talent pipelines, and cross-functional collaboration are the core levers for faster hiring
- AI-powered interviewing and ATS integrations cut time-to-fill without sacrificing candidate quality
- Metrics like time-to-fill, offer acceptance rate, and 90-day retention reveal exactly where your hiring funnel breaks down
Why Healthcare Hiring Falls Behind: The Core Inefficiency Problem
The typical healthcare hiring funnel creates compounding delays at multiple stages. Application review, credentialing verification, multi-round interviews, reference checks, and compliance clearances each add lag time. Filling an experienced RN position takes 83 days on average, while physician searches require a median of 118 days. That's nearly double the cross-industry average of 45-54 days.
The Approval Bottleneck
Healthcare faces a unique "approval bottleneck" that doesn't exist in most other sectors. Clinical hires often require simultaneous sign-off from department heads, infection control, and HR. These multi-stakeholder approval chains create handoff delays that extend timelines by weeks. When credentialing and privileging committees only meet monthly, a single missed meeting can add 30 days to an already lengthy process.
The Candidate Experience Cost
Qualified nurses, allied health workers, and physicians receive multiple offers and accept the fastest reasonable one. 52% of healthcare applicants abandon lengthy applications, with 62% citing excessive length and complexity as the primary reason. When hiring processes drag on, 47% of applicants accept another offer rather than wait for your decision.
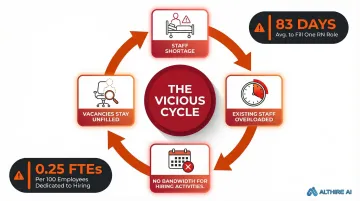
The Vicious Cycle of Understaffing
Understaffing creates a feedback loop that's difficult to break. When clinical teams are short-staffed, existing staff are too busy covering shifts to participate in hiring activities — and hiring managers can't find time to screen candidates or conduct interviews.
The recruiter side faces equal pressure. With an average of just 0.25 recruitment FTEs per 100 employees, healthcare recruiters are already stretched thin. Common realities include:
- Managing 15 to 21 active physician searches simultaneously
- Limited bandwidth to source, screen, and follow up with candidates
- Delays in feedback loops that push qualified candidates toward competing offers
Key Strategies to Improve Healthcare Hiring Efficiency
Standardize and Front-Load Screening
Moving credential verification, license checks, and must-have qualification screening to the earliest stage prevents wasted time interviewing unqualified candidates. A structured pre-screening checklist for clinical roles should verify:
- Active state licensure and expiration dates
- Required certifications (BLS, ACLS, specialty credentials)
- Minimum experience thresholds
- Educational requirements from accredited programs
- Clean background check and drug screening eligibility
Structured interview scorecards with standardized, role-specific questions reduce the time hiring managers spend evaluating candidates inconsistently. This approach also reduces bias in clinical role decisions by ensuring every candidate is assessed on identical criteria.
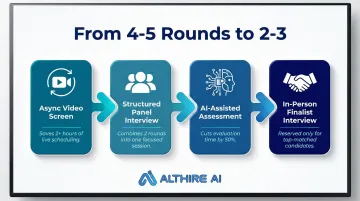
Reduce Interview Rounds Without Reducing Rigor
Healthcare organizations often default to 4-5 interview rounds when 2-3 well-structured rounds with the right stakeholders can yield equally strong hiring decisions. Compress interview stages by:
- Combining initial phone screens with structured video interviews
- Conducting panel interviews with multiple stakeholders simultaneously
- Using asynchronous video assessments for initial screening
- Reserving in-person interviews only for finalists
This compression doesn't cut corners on patient safety criteria—it eliminates redundant conversations and ensures the right decision-makers participate at the right stages. Tightening interview structure also creates space for the other half of hiring efficiency: building candidate supply before roles open.
Build a Proactive Talent Pipeline
Proactive sourcing replaces last-minute vacancy hiring with strategic relationship-building. Build connections with nursing schools, allied health programs, and locum networks before vacancies arise, creating a warm candidate pool ready to deploy immediately.
UW Health's apprenticeship program achieved a 95% retention rate and reduced recruitment time from the 83-day baseline through exactly this kind of internal pipeline development—proof that investment in sourcing relationships pays off before a single vacancy is posted.
Create candidate personas for high-turnover roles like ICU nurses and medical assistants so sourcing strategies and job descriptions are always ready to deploy, rather than built from scratch when a vacancy opens.
Enable Cross-Functional Hiring Collaboration
Involve clinical department heads and charge nurses early in defining role requirements—not just at the interview stage. This eliminates the most common source of late-stage candidate rejection in healthcare: discovering that the candidate doesn't meet unstated clinical expectations or cultural fit criteria that weren't communicated to recruiters upfront.
Practical ways to build this alignment early:
- Hold role-definition sessions with charge nurses before posting any clinical vacancy
- Document non-negotiable clinical expectations in the recruiter brief, not just the job description
- Include at least one clinical stakeholder in scorecard design
- Set a shared definition of "qualified" before screening begins
Leveraging AI and Technology to Accelerate Healthcare Hiring
AI-powered interview platforms solve the scheduling and screening bottleneck that plagues healthcare hiring. Candidates can complete structured interviews on their own schedule, including nights and weekends when healthcare workers are available. This eliminates the back-and-forth that typically delays the process by days or weeks.
Platforms like AltHire AI deliver adaptive, 24/7 AI-conducted interviews with detailed scoring reports. Healthcare recruiters can reduce screening interview time by up to 60% while maintaining consistency across all candidates. The system conducts interviews around the clock, accommodating nurses finishing night shifts or physicians between clinical responsibilities.
Those scheduling gains compound when the rest of the hiring workflow catches up to the same speed.
ATS integrations remove manual work. Modern platforms support 20+ ATS integrations, enabling candidate data to flow automatically from application to assessment to offer. This eliminates manual data entry, reduces errors, and cuts administrative overhead. When interview results sync directly to Greenhouse, Lever, Workable, or BambooHR, recruiters focus on decision-making rather than data transfer.
Bias-free structured scoring matters in healthcare. AI-powered proctoring and objective evaluation criteria are essential for regulated environments. Documented evaluations create an audit trail that supports compliance requirements while ensuring every candidate is assessed on identical criteria regardless of who conducted the evaluation. Question-level precision with AI flags for inconsistencies gives recruiters transparent, data-backed views of candidate performance.
Human judgment remains central. AI handles the repeatable, time-intensive work: scheduling, initial screening, and data capture. Human decision-makers retain full control over final hiring decisions, clinical judgment, and cultural fit. This balance keeps patient safety standards intact while giving recruiters more time for the evaluations that actually require their expertise.
Keeping Compliance and Credential Verification From Slowing You Down
Credentialing and license verification are non-negotiable — but running them in sequence adds weeks you can't afford. Integrate verification workflows in parallel with interviews rather than after. While a candidate progresses through interview rounds, simultaneously verify:
- State licensing board status and expiration dates
- DEA registration for prescribers
- Primary source verification of education and training
- Background screening and immunization records
Build a pre-offer compliance checklist so nothing surfaces post-offer that could derail the hire. Catching gaps before an offer is extended keeps both parties from wasting time.
Timeline benchmarks vary significantly by role:
| Role | Standard Timeline | Complex Cases |
|---|---|---|
| Physicians | 60–120 days | 90–180 days |
| RNs & Allied Health | 1–4 weeks | Varies by source responsiveness |
The biggest delays typically come from payer enrollment (60–120+ days), privileging committee schedules, and slow primary source responses. Counteract these by submitting payer enrollment applications immediately upon offer acceptance and booking privileging committee reviews proactively. Managing these tracks in parallel — rather than queuing them — is often the difference between a 90-day hire and a 150-day one.
KPIs Every Healthcare Hiring Team Should Track
Monitor these core efficiency metrics to identify where your funnel is leaking:
- Time-to-Fill vs. Time-to-Hire — Time-to-fill tracks how long a role stays open; time-to-hire measures your internal process speed. The 83-day average for RN positions and 118-day median for physicians are useful benchmarks, though your numbers will vary by specialty and geography.
- Application-to-Interview Conversion Rate — Below 10-15% suggests unclear job descriptions or overly rigid screening. Above 30% means you're likely interviewing unqualified candidates and burning recruiter time.
- Interview-to-Offer Ratio — A poor ratio often signals misaligned expectations between hiring managers and recruiters, not a shortage of qualified finalists.
- Offer Acceptance Rate — Rates below 75-80% point to compensation gaps, employer branding issues, or candidates taking faster offers from competitors.
- Early Turnover Rate (Within 90 Days) — The first-year RN turnover rate of 22.3% makes this metric impossible to ignore. High 90-day attrition typically signals poor job fit, unrealistic expectations set during hiring, or weak onboarding.

Set Department-Level Benchmarks
Tracking these KPIs at the department level — not just organization-wide — is what separates useful data from noise. Hiring a hospitalist carries very different urgency and pipeline dynamics than hiring a medical coder. Department-level tracking shows exactly where specific teams are struggling and where targeted interventions will deliver the highest return.
Track cost-per-hire alongside time-to-fill to quantify the daily cost of unfilled clinical roles. RN turnover costs an average of $61,110, and modeled daily vacancy costs run around $736 when factoring in agency fees and overtime. Those numbers make the ROI case for faster hiring tools straightforward to bring to leadership.
Frequently Asked Questions
What is the average time-to-hire in healthcare compared to other industries?
RN positions average 83 days to fill; physician searches take 118 days. By comparison, most other industries average 45–54 days. The gap comes down to credentialing and compliance requirements that can't be shortcut.
What are the biggest bottlenecks in healthcare recruiting?
Three bottlenecks drive most of the delay:
- Credential verification: 1–8 weeks for RNs and allied health; 60–180 days for physicians
- Interview scheduling: multi-round coordination compounds delays across departments
- Reactive pipelines: no pre-built talent pool means every vacancy starts from scratch
How can healthcare organizations hire faster without compromising patient safety standards?
Front-load screening to verify credentials early, use structured interview frameworks with consistent evaluation criteria, and run compliance checks in parallel with interviews rather than sequentially. This allows speed and rigor to coexist.
How does AI improve healthcare hiring efficiency?
AI automates scheduling, conducts structured screening interviews 24/7 to accommodate healthcare workers' irregular schedules, and generates objective candidate reports with detailed scoring. This frees recruiters to focus on high-judgment decisions while reducing screening time by up to 60%.
What KPIs should healthcare HR teams prioritize for hiring efficiency?
Focus on time-to-fill by department and role, offer acceptance rate (target 75–80%+), and 90-day retention as the three most actionable indicators. These metrics reveal where candidates drop out and whether hires succeed long-term.
How important is employer branding in healthcare recruitment?
In competitive specialties, employer brand often decides which offer a candidate accepts. Work-life balance and visible career development carry the most weight when candidates are choosing between similar compensation packages.


